|
Orthopaedic surgeons are the main treating surgeon for common foot and ankle traumatic conditions or complex hind foot cases like TAR. Results: We found that the number of foot and ankle procedures performed annually is steadily increasing. We recorded the timing and nature of procedures along with various features associated with the surgeon and the geographic location of the treatment facility. We searched current procedural terminology (CPT) codes for total ankle replacement (TAR), triple arthrodesis, hallux valgus correction, pilon fracture open reduction and internal fixation (ORIF), calcaneus fracture ORIF, and ankle fracture ORIF. 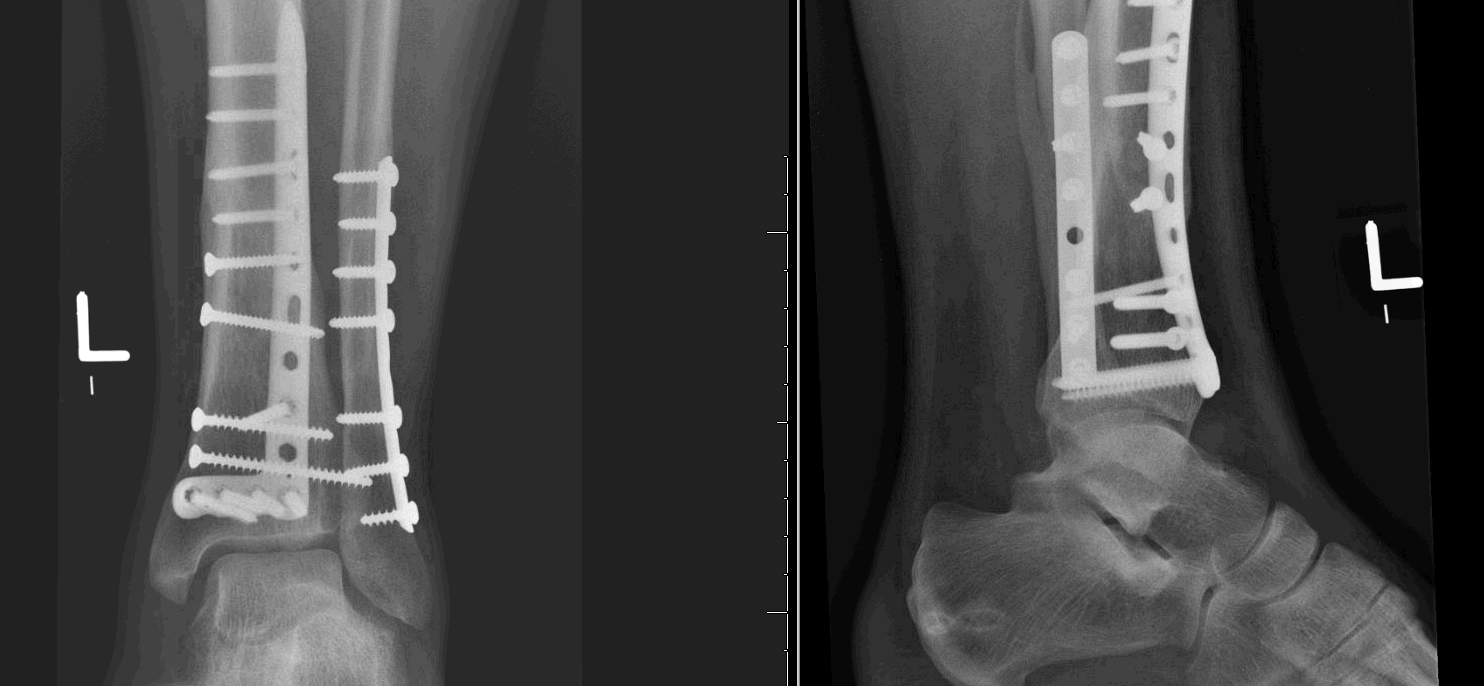
Materials and Methods: A retrospective analysis was performed using the Marketscan Claims Database (Truven Health Analytics, Ann Arbor, Michigan) which covers most privately insured patients under the age of 65 in the USA from 2005 to 2014. With the trend in healthcare now placing increased emphasis on quality and standardizing patient care, this study aimed to characterize the distribution, volume, and trends of certain foot and ankle surgeries performed in the US by both orthopaedic surgeons and podiatrists. Levels of Evidence: Level IV: Case series, Clinical research.Ībstract = "Background: Foot and ankle surgeries in the United States (US) are currently performed by orthopaedic surgeons or podiatrists with specialty surgical training. Discussion: Our study showed the trends in surgical volumes and differences between surgical podiatrists and orthopaedic surgeons and the evolution of these volumes over a ten year period and differences in surgical repertoire between orthopaedists and podiatrists. On the other hand, our study showed that podiatrists perform almost 9 out of 10 hallux valgus correction surgeries. 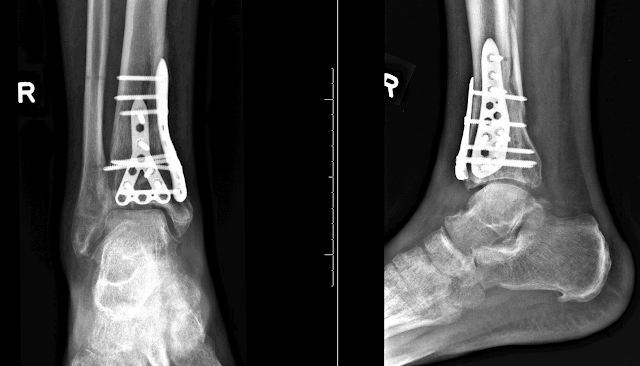
With the proper attention to detail, long-term results will be maximized.Background: Foot and ankle surgeries in the United States (US) are currently performed by orthopaedic surgeons or podiatrists with specialty surgical training. The surgical technique should be well planned for and include the use of meticulous soft tissue techniques and indirect reduction methods. Definitive fixation should be planned for between 10 and 14 days, by which time the soft tissue envelop is likely to be ready to accept the further insult of surgery. Any open would should be addressed at this time. The authors follow the recommendations of Patterson and Sirkin and believe that high-energy pilon fractures should be temporized with an external fixator with or without fibular plating to restore length. Staging the treatment of the patient can minimize development of soft tissue complications. Others believe that open reduction and internal fixation to avoid articular incongruence and development of axial malalignment is needed for good long-term outcome. Some authors think that bridging external fixation with or without limited internal fixation should be employed in high-energy fractures. The high-energy, compression type of fracture has had uniformly moderate results and historically high complication rates. 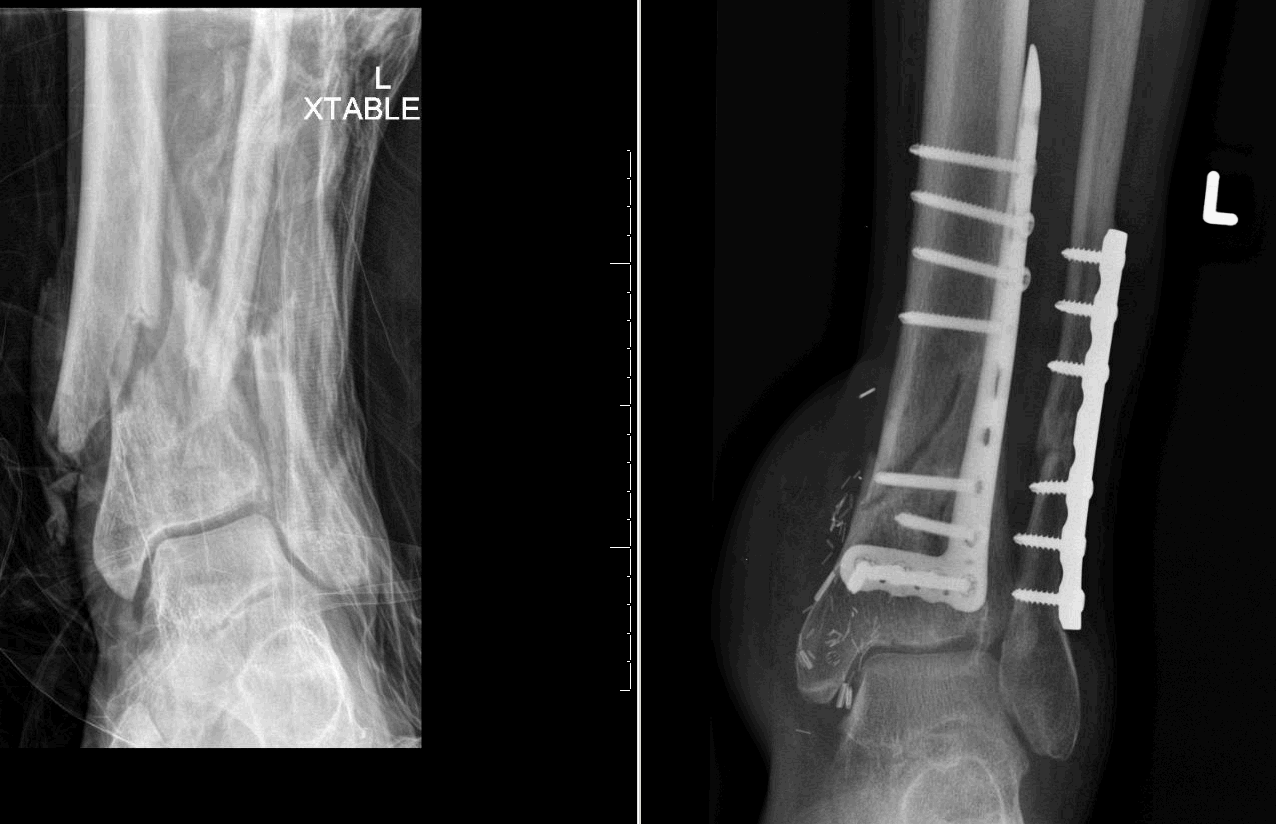 
The low-energy, rotational type of fracture has been shown to have excellent clinical and functional results with open reduction and internal fixation. These injuries generally fall into one of two categories. Although it is evident that the fracture of the tibial plafond is a complex, often debilitating injury, its management is not clear.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
